by Kazeem Olalekan MRPharmS
 The dilemma of Dementia was brought into sharp focus for me recently when I attended the events organised by the Wessex Local Pharmacy Forum. The event took place on the 14th of October at Holiday Inn Eastleigh. Stephen Bleakley, Deputy Chief Pharmacist at Southern Health NHS Foundation Trust and a representative from Hampshire Dementia Action Alliance, Debbie made powerful cases for keeping this at the very top of our professional agenda.
The dilemma of Dementia was brought into sharp focus for me recently when I attended the events organised by the Wessex Local Pharmacy Forum. The event took place on the 14th of October at Holiday Inn Eastleigh. Stephen Bleakley, Deputy Chief Pharmacist at Southern Health NHS Foundation Trust and a representative from Hampshire Dementia Action Alliance, Debbie made powerful cases for keeping this at the very top of our professional agenda.
National Lead:
At a national level, the Department of Health set out a national Dementia challenge in March 2012 led by Prime Minister David Cameron to tackle one of the most important issues we face as the population ages. The key area aims of the strategy are:
- Improve Awareness
- Earlier diagnosis and intervention, and
- Higher quality of care.
The questions I always ask in cases like this is where do I fit into the overall strategy? How will my practice change? How can I make a difference?
The anguish faced by people living with dementia was brought to my door step by the story featured in the Express, where Lady Sally Grylls, mother of that TV adventurer Bear Grylls, described a scenario where frail and elderly patients lay in agony, confused, isolated and terrified with no one to reassure them! She lives in Hampshire & Isle of Wight – my patch!
How can I, as a pharmacist, respond to the challenges posed by Dementia?
I attended the Wessex LPF event for a start!
Stephen Bleakley did a great job in refreshing my memory about the condition. Dementia, he observed, is a progressive degenerative neurological disease. About 800,000 people in UK have Dementia and the figure is expected to double over the next 30 years! The symptoms may include ongoing decline of the brain and its abilities and may include:
- memory loss
- thinking speed
- mental agility
- language
- understanding
- judgement
More information on condition is available on the NHS Choices website.
The types of dementia include:
- Alzheimer’s disease
- Vascular dementia
- Dementia with Lewy bodies (DLB) related to Parkinson’s disease
- Frontotemporal dementia
- Mixed dementia
Stephen Bleakley’s talk introduced us to a Mini Mental state Examination toolkit (MMSE) which is an assessment toolkit most commonly used to test for complaints of memory problems. The Alzheimer’s society has produced a fact sheet the MMSE here. This is of course a validated proprietary tool which is available to buy through Psychological Assessment Resources (PAR).
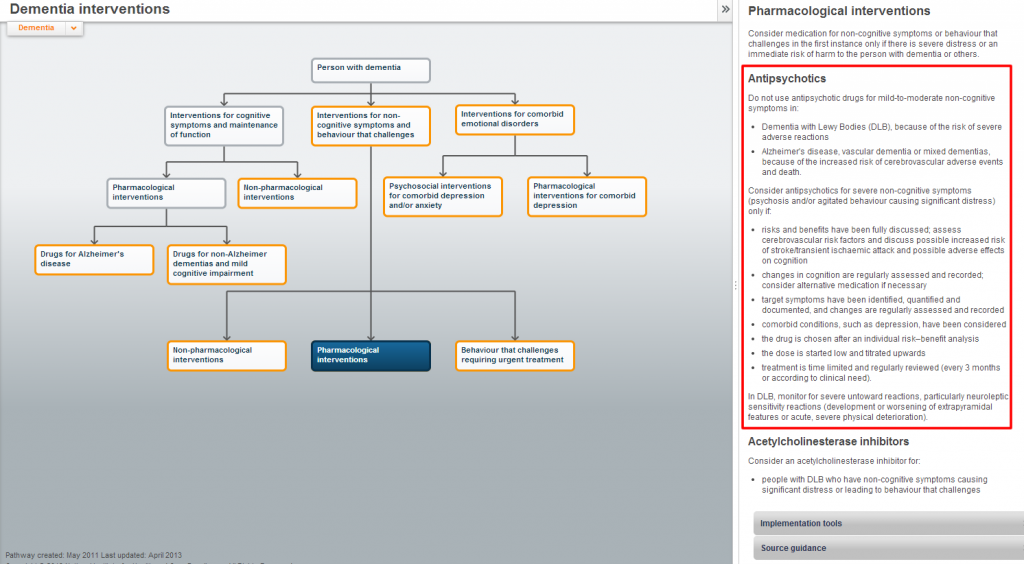
Stephen then went on to describe pharmaceutical agents currently available for managing patients living with dementia:
- Acetylcholinesterase inhibiting drugs such as Donepezil, Galantamine and Rivastigmine
- N-methyl-D-aspartate (NMDA) antagonist sometimes known as glutamate receptor antagonist such as Memantine
There is a NICE guideline (TA217), which discusses the place of each treatment in the management of Alzheimer’s
Stephen further went on to describe the role of other pharmaceutical agents in the management of comorbid symptoms:
- Benzodiazepines may increase the risk of falls
- Anti-depressants have mixed effectiveness and risk vs benefit must be carefully considered
- Mood stabilisers like Carbamazepines and Valproates may be considered where appropriate
As far as managing people with dementia, the best practice is identified in the NICE Dementia Guideline CG42 and Dementia Quality standards.
Apart from the above, how else can we help as pharmacists?
With this post, how is bookapharmacist.com doing it’s bit for Dementia?:
- Improving public and professional awareness and understanding
of dementia - Good-quality early diagnosis and intervention for all
- Good-quality information for those with diagnosed dementia
and their carers - Enabling easy access to care, support and advice following
diagnosis - Development of structured peer support and learning networks
- Improved community personal support services
- Put Dementia on the Pharmacist agenda
At the end of the Wessex LPF event, I interviewed some pre-registration pharmacists. These were their comments:
<end>







Leave a Reply